PsA ja teie organism
PsA ja teie organism
Large joints
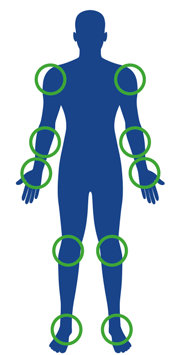
Areas affected

Peripheral arthritis
Peripheral arthritis can affect the large joints,8 such as the shoulders,9 elbows, wrists, knees and ankles,8 causing severe swelling.5 Peripheral arthritis can also involve dactylitis, which is swelling that can affect the fingers and toes, and enthesitis, or inflammation where the tendon or ligament attaches to the bone.8
Small joints
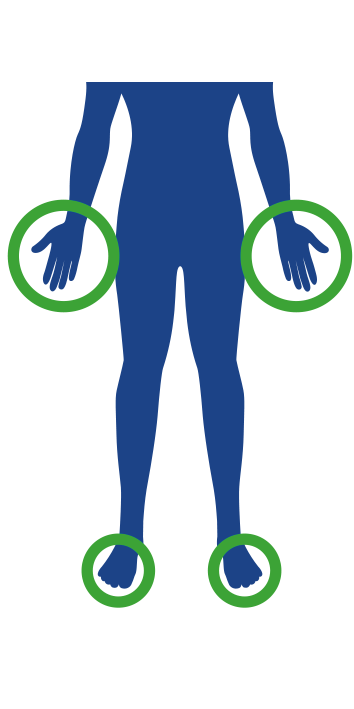
Areas affected
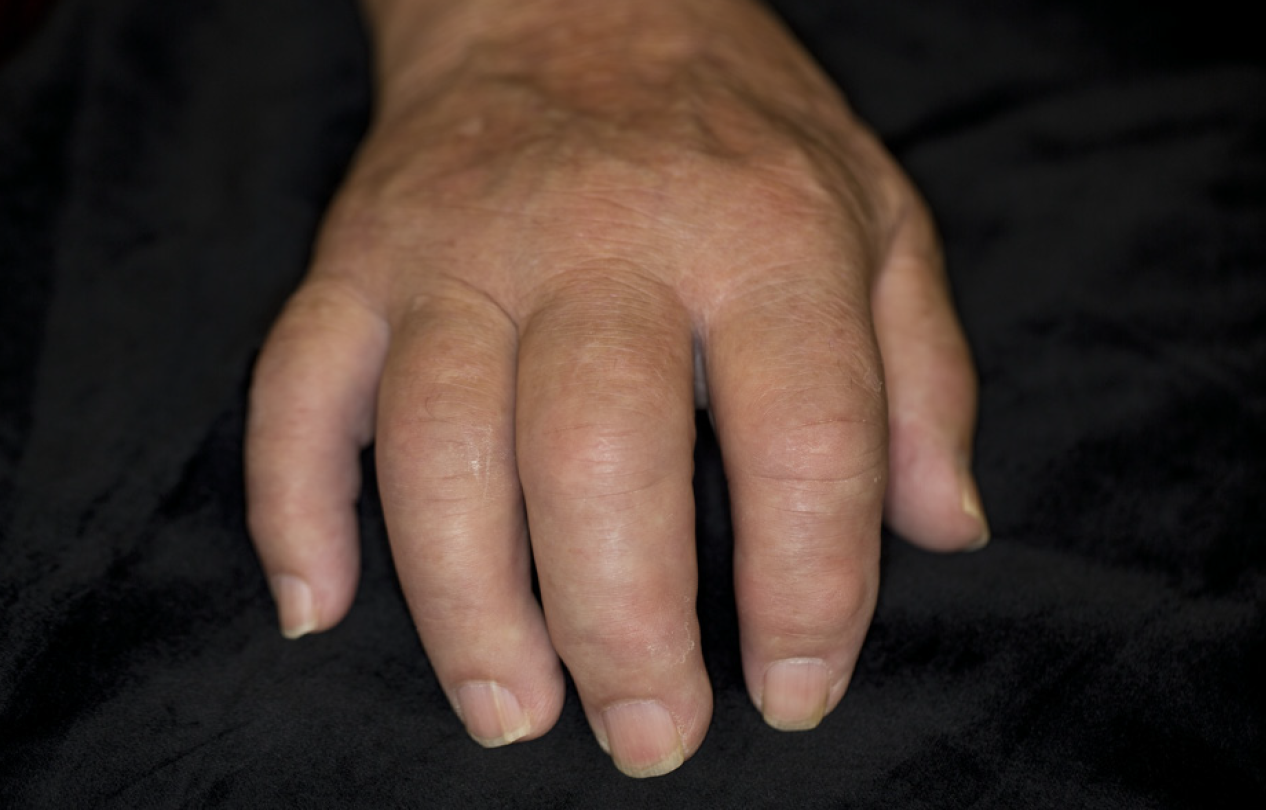
Dactylitis
When a whole finger or toe becomes inflamed and swollen, it’s called dactylitis [pronounced dack-till-eye-tis].10 It can give fingers and toes a ‘sausage’ like appearance,78 which can make them difficult to use and might affect the way you live your life.11 As dactylitis can be the first sign of PsA, if you have it, your doctor may check your skin and nails too, to see if they are affected.8
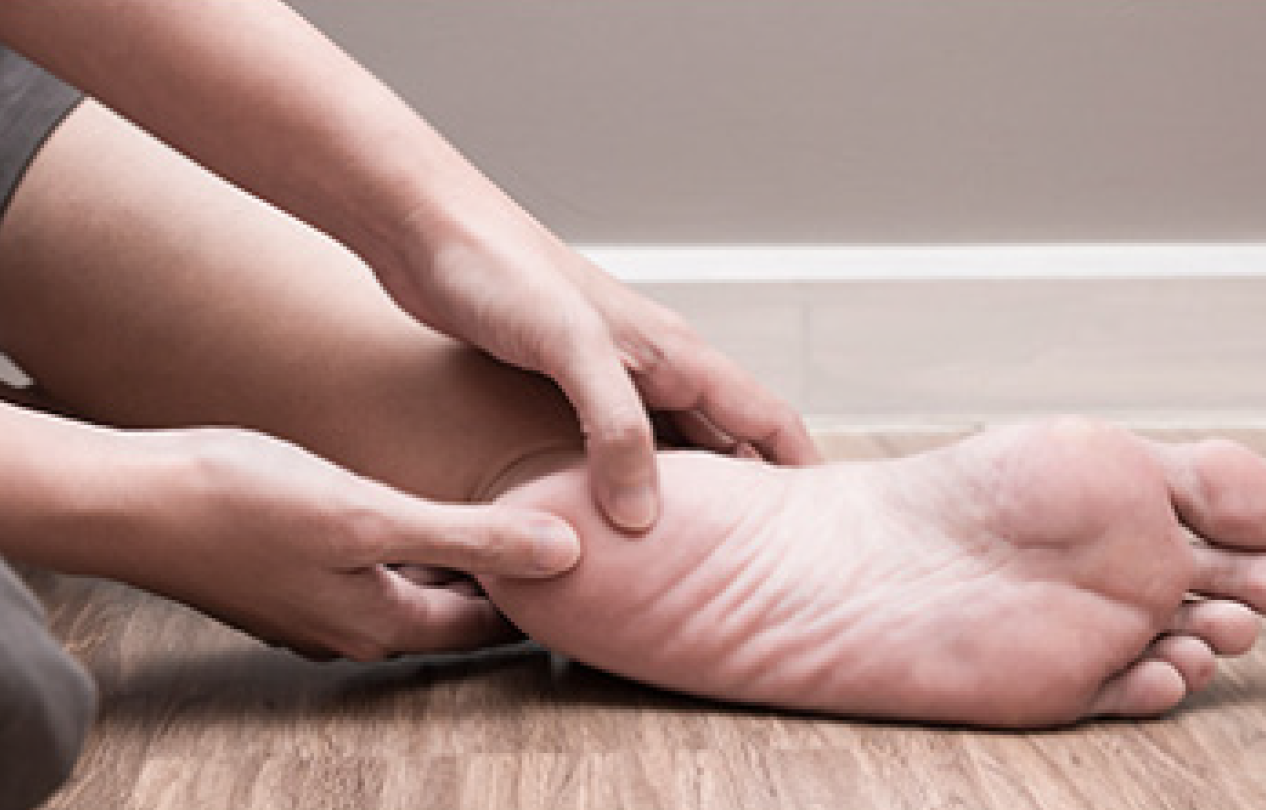
Enthesitis
About half of people with PsA suffer from enthesitis [pronounced enth-ess-eye-tis], or inflammation of the enthesis, where the tendon or ligament attaches to the bone.8 It may happen in many different areas of the body, but it is common around the heels, the bottom of the feet and the elbows.8 If you have enthesitis in your feet, it could make it painful to walk.12
Küüned
Areas affected
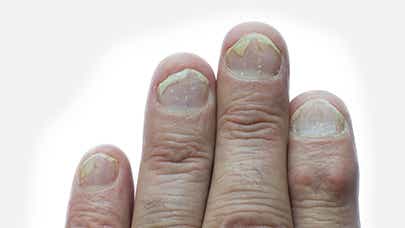
Nail psoriasis
Nail psoriasis happens in about half of people with psoriasis and 80% of people with PsA,13 so it’s worth watching yours in case they start to show symptoms. It can cause changes, such as pitting (indentations) or ridges (lines running from the nail bed to the end), loss of nails, a salmon pink discoloration of the nail,14 called the ‘oil drop sign’, and crumbling of the nail.15 Nail psoriasis is linked to more severe psoriasis and can affect quality of life,16 so speak to your doctor if you think this is true for you.
Skin
Areas affected
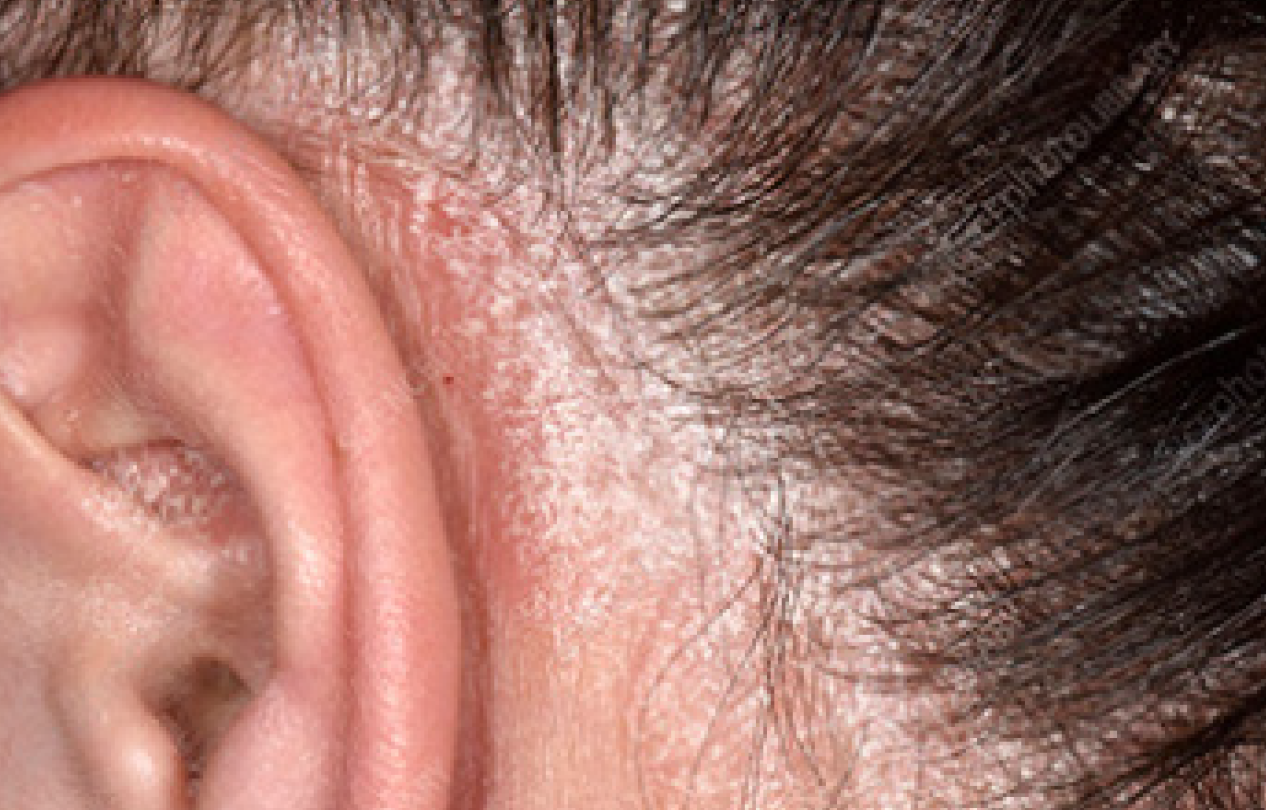
Plaque psoriasis
About 80% of people with PsA may have skin involvement,17 which can cause self-consciousness or embarrassment,18 so if you suffer from this, please remember that you’re not alone. Plaque psoriasis can develop before, during or after PsA does,7 and no one’s experience is exactly the same.8 Plaques can appear anywhere on your body, but sometimes these itchy, painful lesions appear on the knees, elbows, scalp, lower back19 behind the ears and between the buttocks.14 There may only be a few spaced-out plaques, or several larger plaques.14
Spine
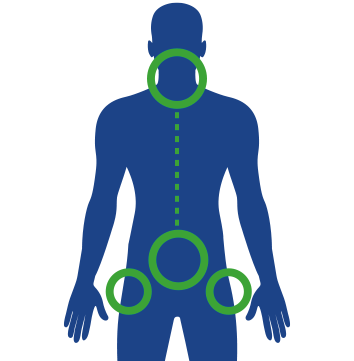
Areas affected

Spinal pain
Spinal pain in PsA6 is caused by inflammation of the spinal column and can affect the neck, lower back and the joints that connect your pelvis and lower spine.20 It can make you feel stiff, make movement difficult20 and even wake you up at night.21 Spinal pain often happens at the same time as other PsA symptoms.20
People with PsA may suffer from one or more of these symptoms – no two patients are alike.8 If you have any questions or concerns about how you’re feeling, be sure to speak to your healthcare professional as there are different treatment options that might help you manage the symptoms2 and help you take control of your life. Before you see your doctor, take a look at some tips for making the most of each appointment.
Kas tahate psoriaasi kohta rohkem teada saada?
Tutvuge psoriaasile pühendatud veebisaidiga, kus on ülevaade ka ravivõimalustest.
Teile võivad huvi pakkuda ka

Nõuanded toimetulekuks PsA peamiste sümptomitega.

Oleme teile allalaadimiseks ette valmistanud mõned lisamaterjalid.

Te pole patsiendina sugugi üksi. On palju teisi inimesi, kellel on samuti psoriaatiline artriit.